 
Operative and non-operative treatments were discussed, and the patient elected to undergo microneurolysis of the median nerve.Ī medial supracondylar incision was made from the medial mid-arm to a point just distal and anterior to the medial epicondyle. Distal humerus (H), olecranon (O).īased on these findings and the lack of improvement in the patient’s symptoms, she was diagnosed with AIN syndrome (AINS). Note the sharp tapering of the fascicle as it approaches the elbow joint, compatible with an intrinsic constriction (solid arrow). 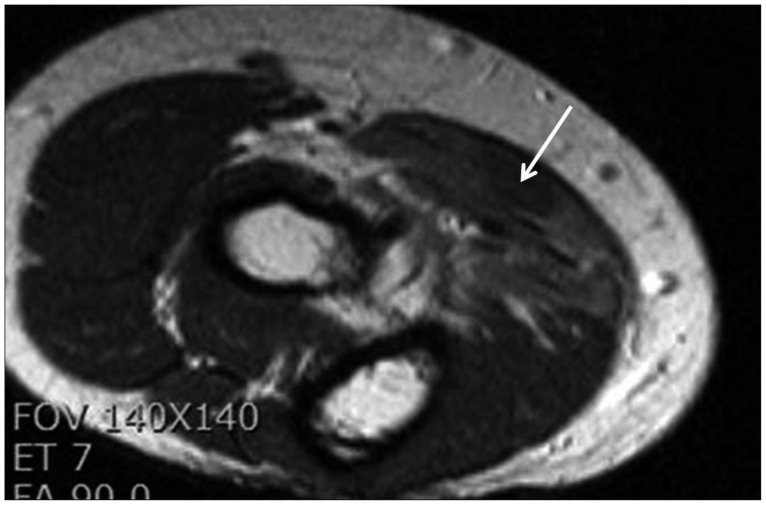
Right forearm ultrasound demonstrated no thickening or contour lobulation of the anterior interosseous nerve (AIN), with some denervation effect seen in the PQ and FPL.įigure 1: Curved, multiplanar reformatted sagittal projection T2-weighted fat suppressed image demonstrates abnormal signal hyperintensity of a posteriorly positioned fascicular bundle (dashed arrows) of the median nerve proper (bracket) within the distal arm. Right forearm MRI demonstrated no extrinsic compression of the median nerve. These fascicles showed focal caliber changes suggestive of fascicular constrictions at the level of the medial epicondyle and within 2 cm proximal to the medial epicondyle (Fig. Magnetic resonance imaging (MRI) of the right brachial plexus demonstrated signal hyperintensity in 2 posteriorly positioned fascicles of the median nerve, approximately 7 cm proximal to the medial epicondyle. The patient also had incomplete denervation of the index FDP, marked by mild abnormal spontaneous activity, nascent voluntary motor unit action potential, and decreased recruitment pattern. The patient otherwise had full strength of all right upper extremity muscles and no sensory deficits.Įlectrodiagnostic testing (EDX) was notable for moderate to severe spontaneous activity, with no voluntary motor activity in the FPL or pronator quadratus (PQ), diagnostic of complete denervation. British Medical Research Council (BMRC) strength grading was notable for M0 strength in the flexor pollicis longus (FPL), M4 strength in the index finger flexor digitorum profundus (FDP), and M5 strength in the long finger FDP. Physical examination showed proximal forearm atrophy, with a positive Kiloh–Nevin sign. She did not recall antecedent arm or forearm pain, although she found it difficult to recall specific symptoms she endured during her severe illness. Her symptoms started 1 week following an episode of septic shock while hospitalized for an acute small bowel obstruction. From Grand Rounds from HSS: Management of Complex Cases | Volume 9, Issue 1 Case ReportĪ 52-year-old right-handed woman presented with 12 months of paralysis of her right thumb. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
